

.
Why Does Polycythemia Cause Headaches?
Feb 14, 2026
Key takeaways
- Headaches in polycythemia vera are often caused by the thickened blood and impaired circulation in small blood vessels.
- These headaches may feel like pressure, throbbing, or migraines, and can worsen after heat, exertion, or dehydration.
- Managing blood counts, staying hydrated, and using medications like aspirin or interferon can relieve symptoms and reduce risks.
Overview
Headaches are a frequent and sometimes severe symptom of polycythemia vera (PV), a condition in which the bone marrow produces an excessive number of red blood cells. This overproduction thickens the blood (a state called hyperviscosity), which slows circulation and makes it harder for oxygen to reach the brain. The result is often pressure-like or throbbing headaches, sometimes accompanied by dizziness or blurred vision [1].
In some patients, these headaches can resemble migraines or cluster headaches, but their cause is quite different; instead of brain chemistry changes alone, they’re linked to poor blood flow and small blood vessels becoming crowded due to an excessive number of blood cells [2].
How do PV headaches differ from regular migraines?
Headaches in PV aren’t caused by the same triggers as regular migraines.
- In PV: The blood becomes thicker than usual, slowing circulation and reducing oxygen delivery to the brain.
- In migraines: The problem is usually nerve sensitivity and changes in brain chemicals.
- That’s why treating PV-related headaches focuses on improving blood flow and controlling blood counts, rather than just providing pain relief.
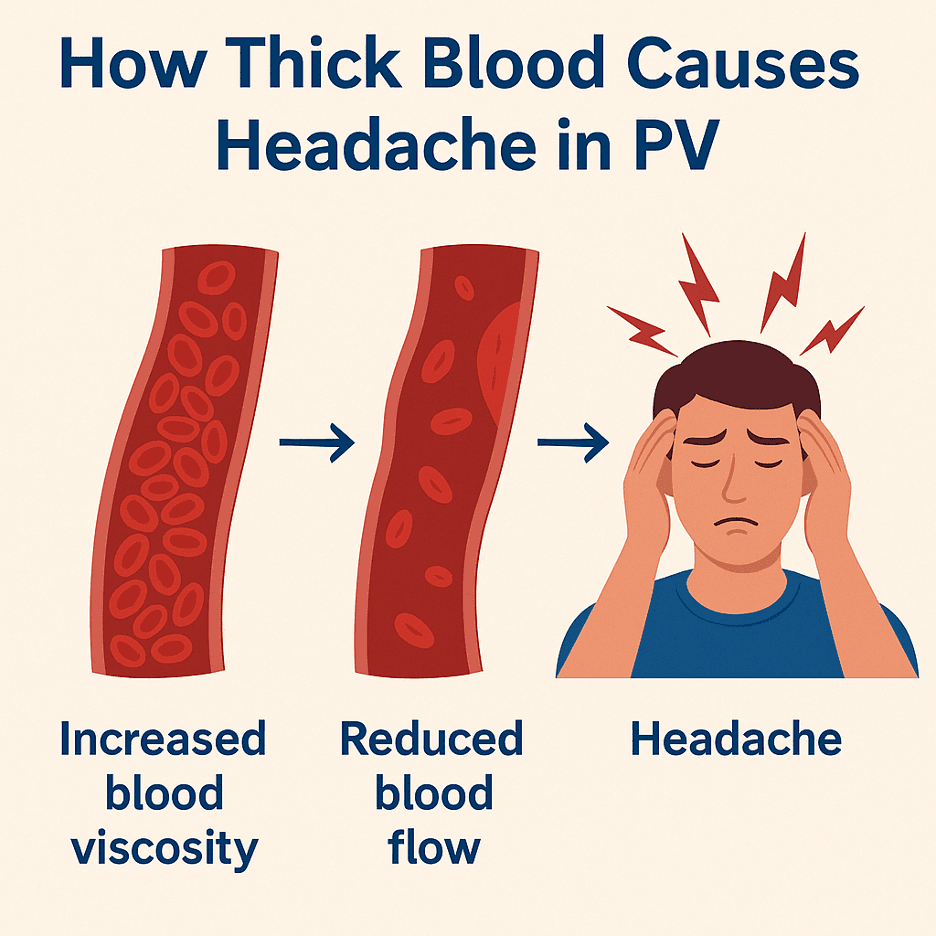
How does polycythemia affect the brain and circulation?
1. Thickened blood (hyperviscosity)
In PV, the hematocrit (the percentage of red blood cells in the blood) is higher than usual, often above 45%, and sometimes much higher. Thick blood moves sluggishly through small arteries and veins, especially those in the brain. This reduced flow can trigger headaches, dizziness, and even blurred vision [3].
2. Reduced oxygen delivery
Even though there are more red blood cells, they may not deliver oxygen efficiently because blood flow slows down. The brain senses this reduced oxygen and responds with blood vessel dilation (widening), leading to a pulsing headache, similar to migraine physiology but caused by blood thickening rather than nerve changes [4].
3. Small vessel and microcirculatory changes
The smallest blood vessels, called capillaries, can become congested when too many cells circulate. This microvascular blockage can explain symptoms such as facial flushing, eye redness, and pounding headaches that often worsen after exposure to heat or bathing [5].
4. Platelet and vascular activity
PV also increases platelet activity (platelets are small cells that help blood clot). When these platelets become too active, they release substances that tighten or irritate blood vessels, leading to headaches or small clots in the brain [6].
How PV-related headaches feel
Patients describe several distinct patterns:
- Pressure or fullness in the head, often worse in the morning or after physical activity.
- Pulsating or throbbing headaches, resembling migraines, sometimes with light sensitivity or nausea.
- Cluster-like pain, with sharp attacks around one eye or temple [2].
- Facial redness and warmth, due to dilated surface blood vessels (a common PV feature called plethora) [5].
While most headaches are benign, new or severe ones should always prompt medical review, as they can also signal high blood pressure, small clots, or increased risk of stroke [1].
Headaches as an early symptom
In some people, headache is one of the first signs of PV, even before blood tests confirm high counts. Case reports describe patients with chronic migraines or unexplained facial congestion who were later found to have PV [2][7]. Because PV develops slowly, it’s common for symptoms like headaches, fatigue, and itching to appear years before diagnosis.
How do doctors manage headaches in PV?
1. Blood count control
- Phlebotomy (blood removal): Reduces hematocrit to <45%, improving circulation and often relieving headaches within days.
- Medications: Low-dose aspirin helps prevent microclots and improves blood flow; cytoreductive agents, such as hydroxyurea or interferon, are used when counts remain high [3].
2. Hydration and lifestyle
Adequate hydration thins the blood naturally. Avoiding dehydration, heat exposure, and long periods of immobility (e.g., flights) can prevent headache flares.
3. JAK inhibitors or interferon therapy
Advanced or symptomatic cases may benefit from disease-modifying drugs that reduce cell production at the cellular level within the bone marrow. These treatments not only help long-term control but can lessen daily symptoms, including headaches [1].
4. Managing triggers
Heat, alcohol, and smoking can worsen headaches by dilating blood vessels or thickening the blood. Limiting these triggers, in conjunction with medical treatment, improves comfort and reduces risks.
When to seek medical help
Seek urgent medical attention if headaches become sudden, severe, or different from usual, especially when accompanied by:
- Vision changes
- Confusion
- Weakness or numbness
- Chest pain or breathlessness
These may signal a blood clot or stroke, which requires immediate treatment.
Final thoughts
Headaches in polycythemia vera are more than a nuisance; they’re a sign that the blood is too thick or not flowing correctly. Fortunately, they often improve once blood counts are brought under control.
Regular monitoring, proper hydration, and use of medications like aspirin or interferon can reduce both discomfort and serious complications. If you live with PV and frequent headaches, discussing symptom patterns with your doctor helps tailor treatment to your needs and prevent long-term risks.
Frequently asked questions (FAQs)
1. Why does PV cause headaches even when blood counts aren’t very high?
Even slight increases in blood thickness or platelet activity can disturb blood flow in the brain’s small vessels. That’s why some people get headaches before their blood counts reach critical levels.
2. Are PV headaches dangerous?
Most are not, but they signal increased blood viscosity or poor microcirculation. In rare cases, they may precede a blood clot or stroke, which is why they should always be reported to your doctor. Seek urgent medical attention if headaches become sudden, severe, or different from usual.
3. Can aspirin really help with PV headaches?
Yes, low-dose aspirin improves blood flow and reduces clot formation in small vessels, which often lessens the intensity and frequency of PV-related headaches.
4. What if phlebotomy doesn’t stop the headaches?
Persistent headaches may mean blood counts are still too high or platelets are overactive. In that case, medications such as hydroxyurea or interferon may be added for improved long-term control.
5. Are PV headaches the same as migraines?
They can feel similar but have a different cause. PV headaches stem from thickened blood and vessel congestion, whereas migraines result from nerve and chemical changes in the brain.
References
- Tremblay, D., et al. (2024). Diagnosis and treatment of polycythemia vera: a review. JAMA.
- Popescu, C. (2020). Cluster-like headache revealing polycythemia vera. Case Rep Neurol, 12(2), 184–188.
- Fox, S., et al. (2021). Polycythemia vera: rapid evidence review. Am Fam Physician, 103(11), 680–687.
- Arregui, A., et al. (1994). Migraine, polycythemia and chronic mountain sickness. Cephalalgia, 14(5), 339–341.
- Razvi, R., & Berman, B. (2023). A teenager with migraines, plethora, and conjunctival injection. Clin Pediatr, 62(1), 77–80.
- Ahmed, S., et al. (2024). Diffuse pulmonary arteriovenous malformation presenting with secondary polycythemia and headaches. J Med Case Rep, 18(1), 313.
- Saxena, P., & Muthu, J. (2022). Challenges of diagnosing headache in sickle cell disease and PV. Blood, 140(Suppl 1), 11154.
Term of Use
The information on this site is provided for general informational purposes only and is not a substitute for professional medical advice. It should not be relied upon instead of guidance from your doctor or other qualified healthcare professional. The content on this website is not intended to be complete or exhaustive.
Always consult your doctor regarding any questions you may have about a medical condition or its treatment, and never ignore professional medical advice or delay seeking it because of something you have read on this website. For further information or advice, please speak with your doctor.